Pulmonary Embolism
Pulmonary Embolism
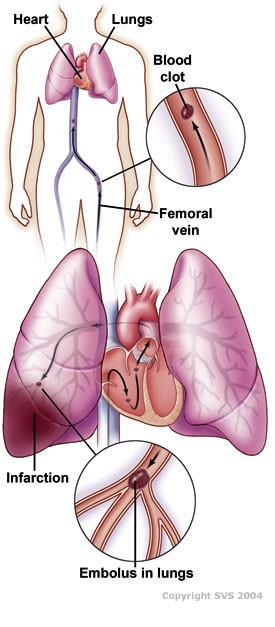
A pulmonary embolism is a blood clot that forms in a vein, travels through your bloodstream, and lodges in your lungs. A pulmonary embolism is a medical emergency because a large embolism, or sometimes many repeated smaller ones, can be fatal in a short time.
Normally, your blood flows from the right side of your heart to your lungs, where it picks up oxygen. The left side of your heart then pumps this oxygen-rich blood through a system of blood vessels called arteries. Once your blood has delivered the oxygen to various parts of your body, it enters another network of blood vessels called the veins. Your veins carry the now oxygen-poor blood back to your heart, which pumps your blood to your lungs to pick up oxygen again. If a blood clot forms in a vein, commonly a deep vein in your leg, it can move with the blood flow back to your lungs and lodge there. This blood clot is called a pulmonary embolism.
If your lung arteries become blocked by a blood clot, you may experience high blood pressure in your lungs. As a result, your heart pumps harder than usual. When your heart is continually overworked, it may enlarge, and it may eventually fail to perform. A large pulmonary embolism can cause your lungs and heart to fail. Fortunately, your chances of surviving a pulmonary embolism increase when your physician can diagnose and treat your condition quickly.
What are the symptoms?
The symptoms you feel can depend on the location and size of your blood clot. Shortness of breath is the most common symptom. Other symptoms include rapid breathing; anxiety and restlessness; chest pain, which might extend into your shoulder, arm, neck, and jaw; coughing or spitting up blood; feeling lightheaded or fainting; and having a rapid heartbeat.
What causes a pulmonary embolism?
The type of clot that is likely to cause a pulmonary embolism usually originates in the veins deep in your muscles. This condition is called deep vein thrombosis (DVT). DVT usually occurs in your leg or pelvic veins; although less commonly it can also sometimes occur in your arm veins.
Factors that increase the risk of DVT or pulmonary embolism include:
What tests will I need?
First your physician asks you questions about your general health, medical history, and symptoms. In addition, your physician conducts a physical exam. Together these are known as a patient history and exam. To confirm the diagnosis of pulmonary embolism, the physician may order specific tests, which may include some of the following:
How is a pulmonary embolism treated?
If you have a pulmonary embolism, your physician or vascular surgeon may administer an anticoagulant drug called heparin intravenously as initial treatment. Anticoagulants are sometimes called blood thinners. They don’t literally thin your blood, but they help prevent your blood from clotting too easily. Heparin helps prevent clots from forming and keeps clots you already have from growing. Eventually, your body breaks up the clot that has caused your pulmonary embolism. Alternatively, a type of medication, called fractionated heparin, may be delivered once or twice daily through an injection in your abdomen. This functions in a very similar fashion to heparin delivered directly into the vein.
If you have a large pulmonary embolism, or you have another medical condition, your physician or vascular surgeon may recommend more aggressive treatments. A treatment called thrombolysis can dissolve your clot. In this procedure, your vascular surgeon injects clot-dissolving drugs through a catheter directly into the clot. A catheter is a long, thin tube that your vascular surgeon inserts into a puncture in the skin over a blood vessel. Thrombolysis has a higher risk for bleeding complications and stroke than anticoagulant therapy but may be effective more quickly, a feature that may be important if the pulmonary embolism is large.
In you are unable to receive anticoagulant therapy or thrombolysis, your vascular surgeon may attempt to remove the clot using a catheter technique. Using this technique, called suction thrombectomy, your physician guides a catheter through your blood vessels to your pulmonary embolism. The catheter shoots a salt solution into the blocked artery. The water pressure pulls the clot toward the tip of the catheter and breaks up the clot. Your vascular surgeon may, as another option, use a catheter attached to a mechanical device such as a rotating head to break up a clot.
Rarely, physicians recommend surgery for a pulmonary embolism. The procedure is called pulmonary embolectomy. You may need this surgery if you have life-threatening blockages in your lungs that are not responsive to other treatments.
Your vascular surgeon will advise you regarding the best treatment option for your particular situation.
Once your pulmonary embolism has been treated, you will usually need to take an anticoagulant drug called warfarin (Coumadin®) for six months or longer to lessen the risk of developing another pulmonary embolism. During the time you are taking medication, your physician will order blood tests to make sure your blood anticoagulation level is adequate to prevent clots but not so high as to cause excessive bleeding. Anticoagulants can cause bleeding problems if the dosage is too high so it is important to follow your physician’s recommendations for testing and dose adjustments.
In some circumstances, your physician may recommend placement of a special metal filter in your main vein, the vena cava, if drug therapy isn’t feasible or isn’t enough to prevent pulmonary embolisms from recurring. This device is called a vena cava filter. The vena cava is a large vein in your abdomen that carries blood back to your heart and lungs. Vena cava filters can trap the clots that break away from your leg veins before they can reach your lungs. You vascular surgeon inserts the filter into your vena cava through a catheter. Some of these filters are left in place permanently and some can be removed. Your vascular surgeon will advise you regarding what is the best option for your particular situation.
What can I do to stay healthy?
Your physician can recommend ways to prevent pulmonary embolisms in the future. These actions include:









