Carotid Artery Disease, Stroke, Transient Ischemic Attacks (TIAs)
What is carotid artery disease?
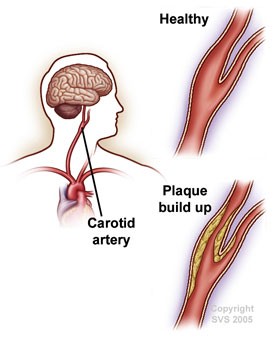
Carotid artery disease occurs when the major arteries in your neck become narrowed or blocked. These arteries, called the carotid arteries, supply your brain with blood. Your carotid arteries extend from your aorta in your chest to the brain inside your skull.
You are more likely to develop carotid artery disease as you age. Only 1 percent of adults age 50 to 59 have significantly narrowed carotid arteries, but 10 percent of adults age 80 to 89 have this problem.
Your arteries are normally smooth and unobstructed on the inside, but as you age, a sticky substance called plaque can build up in the walls of your arteries. Plaque is made up of cholesterol, calcium, and fibrous tissue. As more plaque builds up, your arteries narrow and stiffen. This process is called atherosclerosis, or hardening of the arteries. When enough plaque builds up to reduce or disturb blood flow through your carotid arteries, physicians call this problem carotid artery disease. Carotid artery disease is a serious health problem because it can cause a stroke.
Some plaque deposits are soft and are prone to cracking or forming roughened, irregular areas inside the artery. If this happens, your body will respond as if you were injured and flood the cracked and irregular areas with blood-clotting cells called platelets. A large blood clot may then form in your carotid artery or one of its branches. If the clot blocks the artery enough to slow or stop blood and oxygen flow to your brain, it could cause a stroke. More commonly, a piece of the plaque itself, or a clot, breaks off from the plaque deposit and travels through your bloodstream. This particle can then lodge in a smaller artery in your brain and cause a stroke by blocking the artery.
Fortunately, you may be able to prevent or slow carotid artery disease. Quitting smoking is the most important change you can make to avoid this disease. Other ways to prevent carotid artery disease include:
Controlling factors that increase your chances of developing carotid artery disease, such as diabetes, high blood pressure, or high cholesterol, also help prevent the disease.
What are the symptoms?
Carotid artery disease may not cause symptoms in its early stages.
Unfortunately, the first sign of carotid artery disease could be a stroke. However, you may experience warning symptoms of a stroke called transient ischemic attacks, or TIAs. Symptoms of a TIA usually last for a few minutes to 1 hour and include:
These symptoms usually go away completely within 24 hours. However, you should not ignore them. Having a TIA means that you are at serious risk of a stroke in the near future. You should report TIA symptoms to your physician immediately.
If you experience the above symptoms for longer than a few hours, or they don’t resolve within 24 hours, a stroke has probably occurred. You should contact your physician immediately.
What causes carotid artery disease?
Hardening of the arteries (atherosclerosis) causes most cases of carotid artery disease.
Experts do not fully understand the cause of hardening of the arteries. Plaque may build up in the arteries because of an injury to the artery’s inner lining. Factors that injure artery walls include smoking, high cholesterol, and high blood pressure.
In rare cases, other conditions known as carotid aneurysm disease and fibromuscular dysplasia can also cause carotid artery disease.
Other factors that may increase your chances of developing carotid artery disease include diabetes and having a family history of hardening of the arteries.
What tests will I need?
First your physician asks you questions about your general health, medical history, and symptoms. In addition, your physician conducts a physical exam. Together these are known as a patient history and exam. As part of your history and exam, your physician will ask you if you smoke or have high blood pressure. Your physician will also want to know when your symptoms occur and how often.
During your exam, your physician will listen for sounds of turbulent blood flow in your carotid arteries. He or she may also measure your blood pressure.
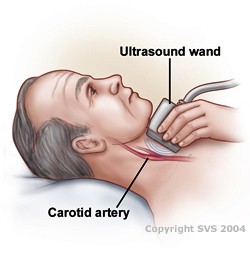
After the history and exam, if your physician suspects you have carotid artery disease, he or she will perform a carotid duplex ultrasound. In this painless test, a technician holds a small ultrasound probe to your neck. The probe emits high-frequency sound waves that bounce off of blood cells and blood vessels to show blood flow and problems with the structure of blood vessels. This test can show your physician how open your carotid arteries are and how quickly blood flows through them.
Carotid duplex ultrasound detects most cases of carotid artery disease. Therefore, your physician usually may not need to perform other tests. However, if ultrasound does not provide enough information, your physician may order one or more of the following:
How is carotid artery disease treated?
Your treatment will depend on the severity of your condition, and whether or not you are having symptoms from the carotid artery disease, as well as your general health. As a first step, your vascular surgeon may recommend medications and the lifestyle changes discussed later in this article.
If you have any other medical conditions, make sure to follow your physician’s instructions to manage them. For example, if you have diabetes, be sure to monitor and control your blood sugar levels. If you have high blood pressure, your physician may prescribe medications to lower it. If you are smoking, you should quit. Have your physician check your cholesterol levels regularly to be sure they stay within normal limits. Your physician may also prescribe medications, such as statins, to reduce high cholesterol.
Surgery
You may require surgery if your carotid artery disease is severe or has progressed. Signs of severe disease include having TIA symptoms, having experienced a stroke in the past, or just having a severely narrowed carotid artery even without symptoms.
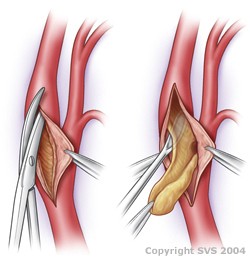
During surgery, your vascular surgeon removes the plaque that is blocking your carotid artery. The procedure is called carotid endarterectomy and can be performed using a local or general anesthetic, depending upon the particular situation. Once the anesthesia has taken affect, the vascular surgeon makes an incision in your neck and then removes the plaque contained in the inner lining of your carotid artery. This procedure removes the plaque and leaves a smooth, wide-open artery. You may even be able to leave the hospital as early as the day after the procedure, depending upon how you feel. This procedure is safe and long lasting when done by a qualified vascular surgeon in the proper circumstances.
Angioplasty and stenting
A newly developed minimally invasive procedure to treat carotid artery disease is angioplasty and stenting. Angioplasty and stenting is usually performed using a local anesthetic. To perform this procedure, your vascular surgeon may insert a long, thin tube called a catheter through a small puncture site over a groin artery and guide it through your blood vessels to your carotid artery. He or she then performs an x ray picture, called an angiogram, by injecting contrast dye through the catheter to show the location and details of the obstructing carotid plaque. The surgeon then inserts another catheter that carries a tiny balloon that inflates and deflates, flattening the plaque against the walls of the artery. Next, the physician places a tiny metal-mesh tube called a stent in the artery to hold it open. Your hospital stay after angioplasty and stenting is approximately the same as with endarterectomy. Carotid angioplasty and stenting is currently controversial because conclusive, long-term results are not yet available. Nevertheless, for patients who have medical conditions that increase the risk of carotid endarterectomy, angioplasty and stenting may be a good alternative. It has been approved for symptomatic patients considered to be at high risk for the surgical endarterectomy procedure, or for patients who have agreed to participate in ongoing clinical studies designed to determine its effectiveness.
What can I do to stay healthy?
If you do not require surgery, make sure you and your immediate family members understand the warning signs of TIA. Follow your physician’s instructions for any prescribed medications, such as aspirin, to thin your blood, or statins, to control your blood lipid (fat) levels. It is also important that you return for any scheduled follow up tests because the carotid blockage may worsen over time, even without warning symptoms.
Changing some lifestyle factors may limit the progression of your carotid artery disease. The first step smokers should take is to quit smoking. Other changes that can decrease your risk of carotid artery disease include losing weight, exercising regularly, and eating a diet low in saturated fats.








